Annual report 2025.
Community Health Impact Coalition is making professional community health workers (proCHWs) the norm worldwide. In 2025, progress took shape across international guidelines, global funding, and national policy.
PROGRESS IN
A YEAR OF PRESSURE.
Dear friends,
2025 was a year of pressure.
Significant cuts to development funding threatened global health progress against a backdrop of climate shocks, rising conflict, and overlapping crises. Governments were asked to expand coverage with fewer resources.
Yet in this constrained financing environment, countries did not retreat from professional community health workers — they increased investment.
At the United Nations General Assembly, Dr. Ouma Oluga, Principal Secretary of Health in Kenya, put it plainly:
“We have found community health to be the foundation of resilient healthcare systems. That is why we have now salaried 107,000 community health promoters. We are not going back.”
Mozambique signaled a similar direction, with Minister of Health Ussene Hilário Isse reaffirming national commitment to professional CHWs at the highest levels of government.
Why?
Because CHWs are one of the only delivery models shown to expand primary care coverage at <$1 USD per capita. In 2025, CHIC published the most comprehensive analysis of CHW program cost-effectiveness to date, covering 10 years of evidence across 380 program scenarios. Across RMNCH, NCDs, HIV, TB, and malaria, CHWs consistently deliver strong outcomes at a median cost of just $0.59 per capita per year.
In a year defined by fiscal contraction, professional CHWs emerged not just as an equity intervention, but as an implementation strategy — enabling governments to maintain essential services, defend workforce investments, and extend care to underserved populations without expanding overall health expenditure.
CHIC’s work in 2025 focused on accelerating this shift: reshaping how global guidance influences financing, how financing enables country action, and how organized CHW leadership sustains momentum across the entire movement.
The proCHW movement did not wait for stability in 2025. It moved anyway because proCHWs are the move for this moment.
As we wrote in TIME this year, progress is not just a question of fortune, but of focus. Join us as an advocate, partner, or supporter in this movement.
With appreciation,
DR. MADELEINE BALLARd
Chief Executive Officer
Community Health Impact Coalition
A VOICE FROM THE
MOVEMENT.
Dear friends,
2025 demanded more from CHWs than many noticed from the outside. It was a year of standing firm, learning fast, and overcoming obstacles. It made clear why we must be seen and heard. Because when systems are fragile, it is CHWs who absorb the shock.
Joining the Coalition in July marked a turning point for me. I learned that we CHWs are not alone. What we experience in Peru—precarity, burnout, lack of support—is shared by colleagues across countries and languages. Exchanging experiences reinforced a hard truth about health systems: when they fall short, we show up.
In 2025, we were asked to deliver more without our working conditions improving at the same pace. We crossed rivers, scaled mountains, and reached communities without basic
services. We faced accidents, violence, and exhaustion. Still, we carried on, because we are the front line that guarantees prevention, health promotion, and real access to care.
On the ground, we call it acompañamiento. It means no one is left behind. It means rebuilding trust and strengthening ties between communities and government. This daily work keeps health systems rooted in the people they serve.
What changed was our conciencia colectiva. We learned that power does not respond to isolated voices. It responds to organized leadership. In 2025, CHWs showed up at local, national, and global forums—not as anecdotes, but as living voices. We named what is happening in our communities and demanded a role in shaping decisions.
We advanced legislative proposals addressing economic incentives, formalization, and the creation of a national CHW association. These efforts represent thousands of compañeras who cannot always be present.
Some things did not change. Too many CHWs still do not know their rights. Harassment continues. The word “volunteer” is used to justify no pay, no equipment, no protection. Without institutional backing, our rights remain fragile.
This year reaffirmed that proper training and decent pay are not privileges. They are minimum conditions for sustainability. A resilient health system cannot be built on the permanent sacrifice of CHWs living in poverty. We cannot be asked to protect life without being protected ourselves.
Looking ahead, progress must be defended. Bills must be passed. CHW organization must grow. Above all, we need a seat at the table.
If 2025 taught us anything, it is this: We only step back to spring forward.
Si retrocedemos, es solamente para tomar impulso. Nuestra voz importa. Our leadership lights the way.
CARMEN VILELA
CHW Leader
Community Health Impact Coalition
Movement
progress.
Despite growing challenges across the global health landscape, the proCHW movement held the line. Rather than losing ground, the sector accelerated. 2025 drove advancements in policy, guidance, financing, and leadership.
Policy momentum
held.
In a year of setbacks, proCHW policy progress held. Countries continued advancing national policies toward salaried, accredited CHWs, even as funding tightened.
2023
countries advanced policy
2024
countries advanced policy
2025
countries advanced policy
COUNTRY POLICY.
- Five governments adopted or strengthened national proCHW policies: Guatemala, Burkina Faso, Côte d’Ivoire, Mauritania, and South Sudan.
- Kenya reaffirmed its commitment, including minimum wage for Community Health Promoters.
- Uganda included payments for 1,400 Community Health Extension Workers in a U.S. government memorandum of understanding.
- Ambitious progress was made to launch proCHW policy dashboard 2.0 by tracking policy and implementation - coming in 2026.
GLOBAL GUIDANCE.
- Peer-reviewed CHIC research informed technical consultations and policy discussions across global institutions:
- 186,329 scholarly article views across peer-reviewed publications where data is available.
- Research on cost-effectiveness, financing visibility, and data systems contributed to a growing norm that healthsystems are strongest when CHWs sit at the center.
GLOBAL FINANCING.
Increase in Global Fund investment for proCHW programs.
Total Global Fund commitment to salaried, skilled, and supplied CHWs.
- The Global Fund reinforced CHWs as “the foundation of resilient and sustainable systems for health,” explicitly recognizing training, remuneration, supervision, and integration.
- Gavi, the Vaccine Alliance publicly elevated the role of paid, trained CHWs in immunization delivery, including through leadership remarks at the World Health Assembly. With framing from CHIC’s CHW immunization impact brief, Gavi called for policies that “must support their training, salaries, safety and integration into formal health systems”.
- The US government’s new America First: Global Health Strategy makes explicit commitments to CHW salaries and benefits as part of its funding portfolio.
- Updated WHO benchmarks and Global Financing Facility guidance increasingly positioned CHWs as legitimate investments in national health and workforce plans.
- For the first time, the World Bank’s goal to extend affordable, quality health services to 1.5 billion more people by 2030, explicitly linked to CHWs’ role in providing care for the hardest-to-reach populations - a keypublic commitment we wanted to achieve in 2025.
ADVANCING CHW LEADERSHIP.
CHW Advocates in the first-ever CHW Speaker Bureau
CHWs have completed the CHW advocates course to date
National CHW Associations
43 CHWs spoke at forums where global health policy is shaped
CHWS attended the 4th International CHW Symposium – the largest virtual gathering of CHWs ever.
HOW CHANGE
HAPPENS.
Changes in community health do not happen in a straight line. We must shift the conditions that hold existing systems in place.

Policies advance,
funding is
committed, and
professional CHWs
are implemented.
Action
Follows.

Clear guidance,
catalytic financing,
and organized
demand reduce risk and unlock action.
Conditions
Shift.
Unclear guidance,
uncertain financing, and uneven pressure
make acting on
proCHW policy risky.
risk shapes
decisions.

Ministries of Health
want stronger
community health
programs.
COMMITMENT
Exists.
CHIC works to shift these conditions through three interconnected tactics.
- Research to equip international norm setters with evidence that informs proCHW guidelines.
- Advocacy to influence global financing institutions to increase and improve funding for professional CHWs.
- Activate to mobilize in-country networks and CHW leadership to win, implement, and sustain proCHW policy.
These tactics reinforce one another and how professional community health workers move from recommendation to reality.
GLOBAL
GUIDELINES.
As resources tightened in 2025, attention shifted from proving the value of CHWs to designing proCHW programs that are cost-effective, accountable, and integrated into health systems. The evidence was already clear: community health workers work.
What decision-makers needed was clarity on what works best, especially in moments of fiscal pressure.
Across peer-reviewed publications, technical guidance, and thought leadership, CHIC offered evidence that supports governments and donors to invest in CHW programs, secure proCHW policy, and build resilient health systems.
FROM FRAGMENTED EVIDENCE TO INVESTABLE MODELS.
For years, economic evidence on community health workers was fragmented - spread across disease areas, countries, and methodologies. Research long showed that CHWs delivered strong outcomes at reasonable cost, but the evidence rarely answered questions governments and funders needed to make sustained investment decisions.
Together, we systematically identified and analyzed every single piece of economic evidence from the last decade, 255 studies covering 380 CHW program scenarios, in the most comprehensive cost-effectiveness analyses of CHWs to date.
The results are unambiguous.
CHWs are a consistent driver of cost-effective care. They’re cost-effective in 8 out of 10 cases for NCDs and mental health, and 9 out of 10 for cases of malaria, HIV, and TB.
The price tag? A median of just 10 dollars per patient per year or just .59 USD per capita for comprehensive primary care - that means everything from vitamin A supplementation to treating cases of malaria, all in one.
When properly supported, CHWs don’t just match facility-based care and alternative delivery models - they outperform them. Consistently. Delivering stronger health outcomes, wider coverage, and better value for every dollar spent.
MAKING PROCHW INVESTMENTS VISIBLE.
Coalition research shows that most funders do not systematically track or report proCHW investments, making it difficult to assess how global health financing reaches CHWs.
Global development financing prior to 2025 included unprecedented levels of investment in health, only a small percentage was directed toward CHWs. From 2007 to 2017, development assistance targeting CHW projects accounted for just 2.5% of total development assistance for health - and even that figure may be overstated.
Transparency shapes how that funding translates into impact. In 2025, CHIC published the first analysis of its kind mapping funding flows for CHWs across eight major global health donors. The analysis highlights a visibility gap.
Without clear, disaggregated data, coordination between governments, donors, and partners suffers. Funding gaps and duplication remain hidden, and alignment with global guidance on proCHW programs is difficult to assess.
Visibility is not just about reporting; it’s about maximizing the impact of every dollar. When CHW funding is visible, donors and governments can align resources, target gaps, and track progress more effectively.
In a constrained financing environment, that visibility is more critical than ever.
FROM FRAGMENTED EVIDENCE TO INVESTABLE MODELS.
For years, economic evidence on community health workers was fragmented - spread across disease areas, countries, and methodologies. Research long showed that CHWs delivered strong outcomes at reasonable cost, but the evidence rarely answered questions governments and funders needed to make sustained investment decisions.
Together, we systematically identified and analyzed every single piece of economic evidence from the last decade, 255 studies covering 380 CHW program scenarios, in the most comprehensive cost-effectiveness analyses of CHWs to date.
The results are unambiguous.
CHWs are a consistent driver of cost-effective care. They’re cost-effective in 8 out of 10 cases for NCDs and mental health, and 9 out of 10 for cases of malaria, HIV, and TB.
The price tag? A median of just 10 dollars per patient per year or just .59 USD per capita for comprehensive primary care - that means everything from vitamin A supplementation to treating cases of malaria, all in one.
When properly supported, CHWs don’t just match facility-based care and alternative delivery models - they outperform them. Consistently. Delivering stronger health outcomes, wider coverage, and better value for every dollar spent.
MAKING PROCHW INVESTMENTS VISIBLE.
Coalition research shows that most funders do not systematically track or report proCHW investments, making it difficult to assess how global health financing reaches CHWs.
Global development financing prior to 2025 included unprecedented levels of investment in health, only a small percentage was directed toward CHWs. From 2007 to 2017, development assistance targeting CHW projects accounted for just 2.5% of total development assistance for health - and even that figure may be overstated.
Transparency shapes how that funding translates into impact. In 2025, CHIC published the first analysis of its kind mapping funding flows for CHWs across eight major global health donors. The analysis highlights a visibility gap.
Without clear, disaggregated data, coordination between governments, donors, and partners suffers. Funding gaps and duplication remain hidden, and alignment with global guidance on proCHW programs is difficult to assess.
Visibility is not just about reporting; it’s about maximizing the impact of every dollar. When CHW funding is visible, donors and governments can align resources, target gaps, and track progress more effectively.
In a constrained financing environment, that visibility is more critical than ever.
“0% of funders fully disclose proCHW specific funding.”
Coalition analysis, BMJ Global Health (2025)
DATA THAT STRENGTHENS SYSTEMS.
Evidence does not translate into better care if it cannot be used.
Data plays a crucial role in the success of CHW programs. It supports the identification of health trends, monitoring of program outcomes, and allocation of resources where they are most needed.
Yet across community health systems, there are core gaps in our understanding of what data is most relevant to inform funders, policymakers, and CHW program managers.
To address these gaps, members of CHIC undertook a thorough overview of current data use within CHW programs.
As part of this effort, CHIC launched the CHW Data Dialogues podcast series in 2025 to explore how data collection, analysis, and use can better support community health systems. Through conversations with implementers, funders, and CHW leaders, the series explored what effective CHW data systems need to do, not only to measure outcomes, but support supervision, strengthen quality of care, and enable integration within national health systems.
Insights from the series shaped a data guide for funders that outlines key lessons and a comprehensive set of recommendations to invest in CHW systems.
As global institutions increasingly emphasize accountability and system performance, this body of work serves as connective tissue linking CHWs, supervisors, facilities, and policymakers in ways that support quality care and durable community health systems.

GLOBAL FINANCING AND
INSTITUTIONAL ADVOCACY.
Evidence clarifies what works and where gaps remain. Advocacy determines whether institutions change course.
In 2025, CHIC focused advocacy efforts where institutional decisions would shape country-level possibilities, especially in a constrained funding climate.
Even amid major aid cuts and pressure on global health financing, momentum for proCHWs deepened, marked by new and sustained commitments from global funders.
GLOBAL FUND INVESTMENT IN CHWS.
In 2025, the Global Fund increased its funding for proCHW programs by 32%, bringing total investment to over US$900 million.
This increase included contributions through a catalytic investment to Africa Frontline First (AFF), where aligned partnerships and private capital helped unlock additional Global Fund resources.
In the 12 months preceding this increase, CHIC submitted technical inputs, convened side events with funder leadership, and provided financing briefs that informed grant design discussions.
The significance of this shift went beyond the funding amount. The Global Fund explicitly recognized CHWs as “the foundation of resilient and sustainable systems for health,” with financing tied to ensuring CHWs are salaried, skilled, supervised, supplied, and fully integrated into primary health care teams.
This framing strengthened the ability of countries and partners to align grant design with national community health strategies and to defend professional CHW investments within constrained budgets.
“Governments need to recognize community health workers and we want to be professionalized.”
CHW Millicent Miruka in conversation with Dr. Sania Nishtar, CEO, Gavi the Vaccine Alliance at CHIC’s WHA78 side event.
RECOGNIZING THE WORKFORCE BEHIND IMMUNIZATION.
At the Seventy-eighth World Health Assembly, discussions on financing, efficiency, and accountability reminded us that CHWs are essential to realizing a first-class health system worldwide.
Throughout WHA78, CHWs were consistently framed as part of the solution to economic downturns, climate change, pandemic risk, and the growing burden of non-communicable diseases. As a coalition, our key message was clear: investing in professional CHWs - who are salaried, skilled, supervised, and supplied - is simple, low-cost, and effective.
That message was reinforced publicly by Dr. Sania Nishtar, CEO of Gavi, the Vaccine Alliance, who underscored the central role that CHWs play in delivering care:
“It is community health workers who have the knowledge and the expertise, and who have the trust…it is them who take primary healthcare to the last mile.”
Public leadership from Gavi signaled that coverage is only possible when the workforce is funded.
RECOGNIZING THE WORKFORCE BEHIND IMMUNIZATION.
At the Seventy-eighth World Health Assembly, discussions on financing, efficiency, and accountability reminded us that CHWs are essential to realizing a first-class health system worldwide.
Throughout WHA78, CHWs were consistently framed as part of the solution to economic downturns, climate change, pandemic risk, and the growing burden of non-communicable diseases. As a coalition, our key message was clear: investing in professional CHWs - who are salaried, skilled, supervised, and supplied - is simple, low-cost, and effective.
That message was reinforced publicly by Dr. Sania Nishtar, CEO of Gavi, the Vaccine Alliance, who underscored the central role that CHWs play in delivering care:
“It is community health workers who have the knowledge and the expertise, and who have the trust…it is them who take primary healthcare to the last mile.”
Public leadership from Gavi signaled that coverage is only possible when the workforce is funded.
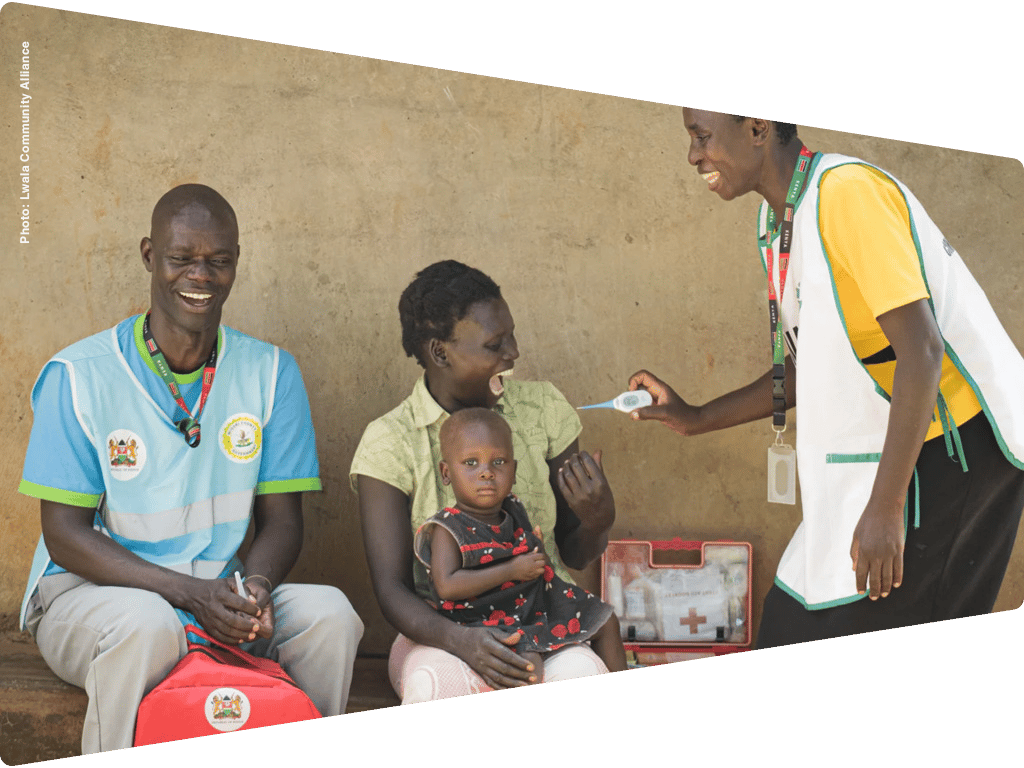
“In the face of economic downturns, political instability, climate change, armed conflict, and pandemic risks, investing in professional CHWs—who are salaried, skilled, supervised, and supplied—is a strategic decision.”
Julius Mbeya, Lwala Community Alliance
EMBEDDING PROFESSIONAL CHWS IN GLOBAL FINANCING FRAMEWORKS.
Global guidance shapes financing norms—and in 2025, those norms moved closer to professional CHW models.
Updated WHO Benchmarks for Strengthening Health Emergency Capacities directly recognized paid, trained, and supervised CHWs as essential to resilient systems, including CHIC inputs on public health and social measures.
Global Financing Facility (GFF) guidance increasingly positions CHWs as legitimate investments within national health and workforce plans.
When professional CHWs and the systems that support them are included in global benchmarks and financing guidance, governments and partners have clearer justification to align funding, defend workforce investments, and move proCHW policies from commitment to implementation.

“In Mozambique, we have a strong political commitment from the President of the Republic. The community subsystem is considered a pillar of government. These community workers have a major role in prevention and promotion within primary healthcare.”
Hon. Ussene Hilário Isse, Minister of Health, Mozambique
COUNTRY POLICY AND
CHW LEADERSHIP.
Policy change is where proCHW practice shapes the lives of CHWs and their patients.
In 2025, CHIC mobilized in-country networks to win national proCHW policy and sustain gains when conditions shifted.
REACHING THE HALFWAY POINT.
Our goal is to see 95 low- and middle-income countries adopt proCHW policies.
In 2025, five countries adopted or strengthened national policies recognizing professional CHWs: Guatemala, Burkina Faso, Côte d’Ivoire, Mauritania, and South Sudan.
2025 ends with 50 countries recognizing CHWs as accredited, salaried professionals in national policy. This marks passing the halfway point to our goal. Now is the time to double down and secure this change for all CHWs, everywhere.
The road to 95.
50 countries recognize CHWs in national policy
To support this work, CHIC stewards the largest public-facing dashboard of proCHW policy adoption.
The Policy Dashboard is a shared resource used across the movement to track policy windows, compare approaches, and guide strategic mobilization. An updated version is planned for 2026 to not just track policy but implementation and whether countries are actually meeting minimum standards for professional CHWs.
DEFENDING AND ADVANCING COMMITMENTS.
Policy changes are rarely final.
In 2025, eight national NGO coalitions played a critical role in shaping and defending proCHW commitments. Coalitions engaged in active policy processes in DRC, Mozambique, and Peru, contributing evidence and coordinating CHW participation.
In Kenya, Uganda, and Malawi, coalitions mobilized to defend existing proCHW commitments amid political transitions and budget pressures - ensuring progress was not quietly rolled back.
Defending commitments in Uganda.
As funding pressures mounted, the Uganda National NGO Coalition, alongside the national CHW Association, engaged Parliament to defend and advance financing for professional CHWs. With strategic support and technical inputs from CHIC, the coalition reinforced the case for sustained public investment.
The result is a national budget commitment to fund accredited and paid Community Health Extension Workers (CHEWs) as part of Uganda’s formal health system.
These efforts showed that sustained alignment—not one-time announcements—is what keeps professionalization on track.

NOTHING ABOUT CHWS WITHOUT CHWS.
For too long, discussions about community health workers have been happening without community health workers. In 2025, that continued to change.
CHWs are vital to the proper functioning of primary healthcare systems, and they will no longer be excluded from policy discussions and decision-making about issues that affect their work, their patients, and their communities.
Through CHIC’s CHW Speaker Bureau, CHWs spoke directly in high-level forums where community health is discussed. Whenever CHWs are talked about, a CHW must be in the room.
At the United Nations General Assembly, Margaret Odera addressed global leaders onstage at the Gates Foundation Goalkeepers event. She shared the consequences of underfunding community health and the need for professional, salaried CHWs who are trained, supervised, and supplied.
That same shift was visible at CHIC’s UNGA side event, where Carmen Vilela Vargas, a lead CHW from Peru, closed with a clear call grounded in organizing and lived experience:
“This is a call for change. Enough of volunteer work. Community health agents, we must organize. For those who aren’t here, for those who are here, and for those who will come.”
To make this possible at scale, CHIC created the CHW Speaker Bureau - the first global registry of CHWs ready to take on speaking engagements—removing barriers to inclusion and streamlining access for conveners. Today, CHWs are no longer only delivering care. They are shaping the conversations and decisions that govern it.
Nothing about CHWs without CHWs.
ORGANIZED CHWS STRENGTHEN POLICY IMPLEMENTATION.
As proCHW policies advanced, CHWs organized to sustain them.
Policy change is only durable when community health workers are organized and able to engage government with a unified, recognized voice. CHIC supports CHWs in building and strengthening their own national associations—rooted in local context and anchored within Ministries of Health.
In 2025, CHW associations were active or emerging in over 10 countries. New CHW organizers were onboarded in the Democratic Republic of Congo and Peru, strengthening coordination between CHWs, civil society coalitions, and government counterparts.
Uganda reached a milestone with the formal registration of a national CHW association. Marking the first time CHWs have a legally recognized platform to engage ministries and partners on workforce policy, implementation, and accountability.
Associations amplify coordinated advocacy, and sustained engagement beyond individual policy moments. They help ensure that professional CHW commitments—around pay, training, supervision, and supplies—are implemented, defended, and improved over time.
Policy change does not end when a document is signed. Organized CHW leadership supports moving from policy to implementation.
Strengthening policy in Guatemala.
Organized CHWs in Guatemala did not wait for policy. Through their national association, the Movimiento Nacional de Abuelas Comadronas Nim Alaxik, they shaped the National Midwifery Policy to secure formal recognition and economic incentives. Leaders then carried that work into implementation, engaging government stakeholders to reinforce regional coordination and accountability.

KEEPING MOMENTUM
WHEN CONDITIONS ARE HARD.
In 2025, progress came from a movement that didn’t pause when the ground shifted. That’s what’s making proCHWs the norm.
As the movement enters its next phase, the work ahead is not about proving the model, but protecting and extending it. The foundation is in place. The responsibility now is to stay aligned, stay accountable, and keep moving forward - together.
MEET
CHIC.
Our dedicated team at the CHIC backbone sets the guardrails for radical collaboration and enables progress towards making proCHWs the norm worldwide. Radical collaboration means that Secretariat growth has a “leverage” effect for the Coalition and the field: as we reinforce our backbone, we invest in tapping the shared expertise of dozens of members, hundreds of allies, and thousands of CHWs who are ready and eager to advance our shared mission.
PRESS.
AWARDS.
- Schwab Foundation for Social Entrepreneurship
Collective Social Innovation Award
- Skoll Foundation
Skoll Award for Social Innovation
AWARDS.
- Schwab Foundation for Social Entrepreneurship
Collective Social Innovation Award
- Skoll Foundation
Skoll Award for Social Innovation
PRESS.
FINANCIAL
OVERVIEW.
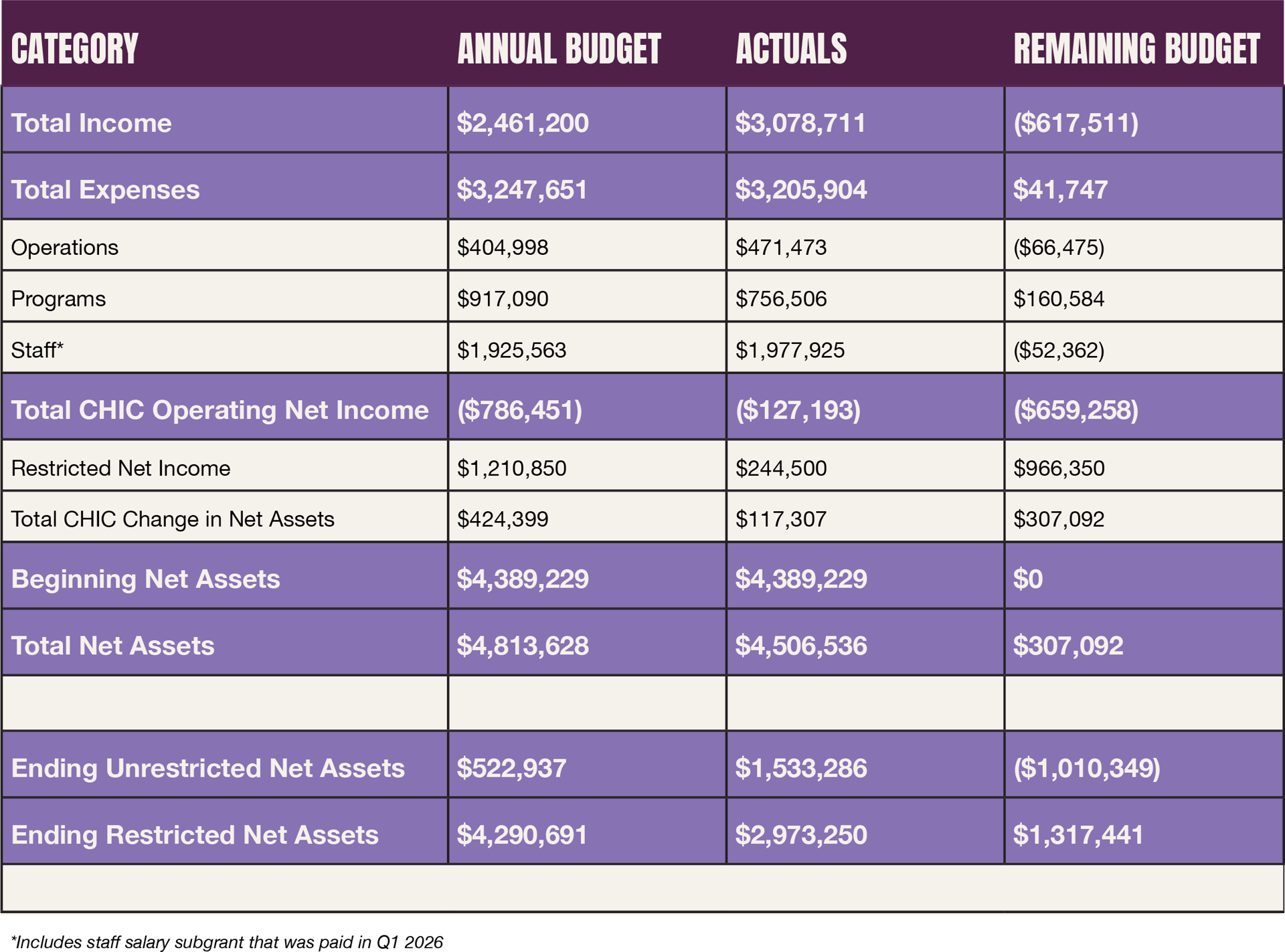
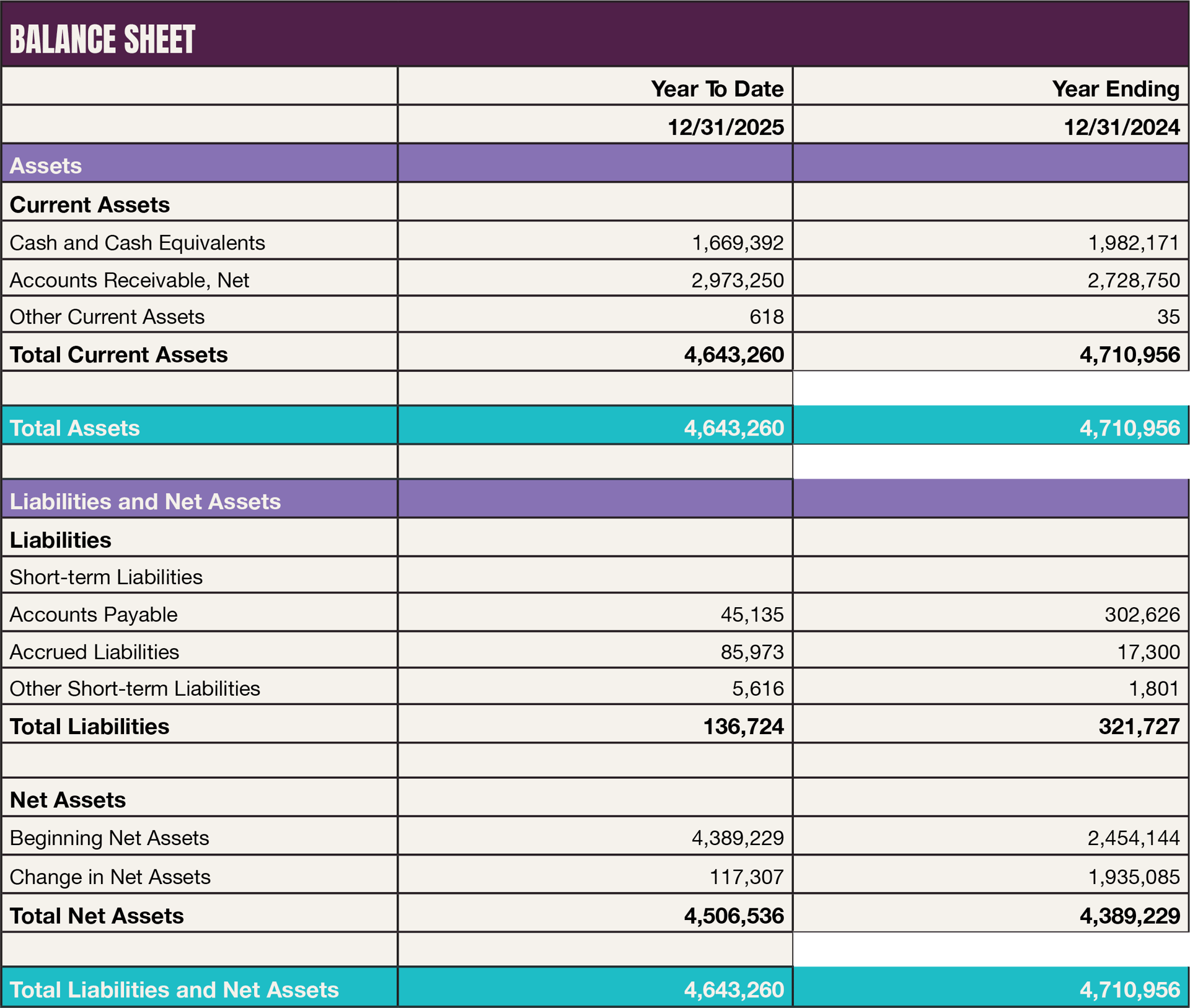
Income and expense statement.
CHIC increased programmatic deployment while maintaining healthy operating reserve in a year of sector-wide retrenchment:
Our 2025 income came in ahead of target at $3,078,711 and we maintained a 4-month cash reserve while increasing year-over-year expenses by 30% from 2024 (N.B. includes a deferred subgrant disbursement to fund 1 FTE 2025 salary).
MEMBERS.



































ALLIES.




































Funders.



















ADVISORY BOARD.

Ari Johnson
Muso

Ash Rogers
Lwala Community
Alliance

Benard Aketch Otieno
CHW, Kenya

Claudia Shilumani
Africa CDC

Dan Palazuelos
Partners in Health

George Mwinnyaa
Johns Hopkins University

Joy Ncomile Ruwodo
Feel the Joy

Jennifer Schechter
Integrate Health

Mallika Raghavan
Last Mile Health

Maryse Kok
Royal Tropical Institute

Naomi Njeri Monobolu
African Development
Bank

Ryan Schwarz
MassHealth

Uzo Osikhena
The Lisben Group
SECRETARIAT.

Dr. Madeleine Ballard
CEO

Carey Carpenter
Westgate
COO

Dr. James O’Donovan
Director of Research,
Digital Innovation and AI

Theebika
Shanmugarasa
Director of Advocacy Mashego

Dr. Lennie Kyomuhangi
Bazira
Director of Policy

Linley Kirkwood
Director of Finance and
Operations

Abby Overton
Communications Lead

Abhijit Dhillon
Advocacy Coordinator

Alexander Wheeler
Senior Development
Manager
Carolyne Faith
Wanyonyi
CHW Engagement
Manager
Deborah Wangia-Okoth
Technology Manager

Francisco Domínguez
CHW Engagement Lead

Kouao Ahoussi
Ferdinand
CHW Engagement Lead

Leah Manickam
Operations Assistant

Shemali Jayasinghe
Executive Assistant

Tumi Mashego
Operations Lead
